Post by unlawflcombatnt on Nov 8, 2009 16:15:38 GMT -6
Below is a link and a list of some changes made to the latest health care reform bill, HR 3962, that differ from the original HR 3200 legislation. This does not include all of the changes, and they are current only through October 29, 2009. Changes made after that time, such as the Stupak Amendment, are not included. This is the official summary of the "TOPLINE" changes from the House Energy and Commerce committee. I have, however, omitted as much of the Obama Administration's talking point propaganda as possible.
energycommerce.house.gov/Press_111/health_care/hr3962_TOPLINE.pdf
"
TOPLINE CHANGES FROM INTRODUCED BILL TO BLENDED BILL
This document is a list of the major policy changes between the Affordable Health Care for America Act (10/29/09) from the introduced HR 3200 bill (7/19/09); it does not include every change....
TOP TIER CHANGES....
Modifies the Income Thresholds and Rates for the Surcharge. In the introduced bill, the surcharge applied to adjusted gross income in excess of $350,000 (married filing a joint return) and $280,000 (single), at rates ranging from 1% to 5.4%. Under the blended bill, the surcharge applies to adjusted gross income in excess of $1 million (married filing a joint return) and $500,000 (single), at a rate of 5.4%.
Public Health Insurance Option. Modifies policy so that the Secretary shall negotiate rates with providers that participate in the public plan and provides greater clarity regarding the opt-out policy for providers.
Physician Payment Reform. Removes overhaul of the Medicare physician payment formula (SGR), which will be permanently reformed by separate legislation this year.
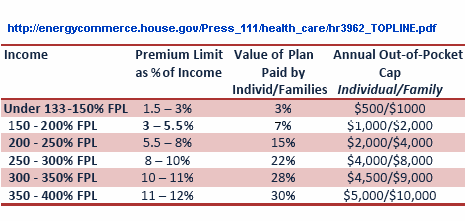
Affordability Credits. In order to reduce the cost of the new coverage to meet the $900 billion goal, affordability premium credits have been scaled back to reflect an amendment adopted by the Committee on Energy & Commerce. Individuals and families between 150% and 400% of FPL [Federal Poverty Level] will pay a larger share of health premiums over time compared to HR 3200 as introduced. Also, the exception for individuals and families with employer coverage who can receive affordability credits in the Exchange is increased to 12% of income. Specific out-of-pocket maximums are added to protect individuals’ level of cost sharing at each income tier (specified below).
----------------------
Page 2
Medicaid. Raises threshold for mandatory Medicaid coverage from 133% of poverty to 150%. Retains 100% federal matching rate for costs of expansion populations in 2013 and 2014, then reduces rate to 91 percent in 2015 and beyond. Deletes provision allowing recently uninsured childless adults with incomes under 133% of poverty to choose between Medicaid and the Exchange. Increases assistance to states that maintain access to Medicaid services during the recession by extending the current Recovery Act increase in federal Medicaid payments to states with high unemployment rates.
Begins Closing the Medicare Part D Donut Hole Immediately. Effective January 1, 2010, closes the Part D donut hole by $500 and institutes a 50% discount for brand-name drugs in the donut hole. Gap in coverage is completely eliminated by 2019.
Secretarial Negotiation of Drug Prices in Medicare. Secretary of HHS is required to negotiate drug prices on
behalf of Medicare beneficiaries.
Addresses Geographic Variation in Health Spending. Instructs the IOM to study the extent and cause of geographic variation in spending on health care (including all payers). The study will focus on major contributors to that variation such as input prices, health status, socioeconomic factors, and access to services. The IOM will make recommendations to the Secretary, and the Secretary will submit to the Congress an implementation plan to appropriately address such variation in Medicare. To the extent the plan would result in dramatically different payments, it must take into account the need to maintain beneficiary access to
services and minimize disruption for providers. CMS will implement changes to Medicare payment systems unless Congress votes to disapprove the planned changes.
Establishes a Center for Medicare & Medicaid Innovation. Creates a Center for Medicare & Medicaid Payment Innovation within CMS not later than 2011 to test and expand new payment models that encourage higher quality and lower cost.
CLASS Act. Creates a new, voluntary, public, long-term care insurance program to help purchase services and supports for people who have functional limitations. After a contribution period, individuals determined to need assistance because of functional limitations would qualify to receive a daily or weekly cash benefit to help purchase the services and supports needed to maintain personal and financial independence. CLASS would supplement, not supplant, traditional payers of long-term care (e.g. Medicaid and/or private long term care insurance).
Immediate Sunshine on Price Gouging (Rate Review). Discourages excessive price increases by insurance companies through review and disclosure of insurance rate increases and rationale for such increases.
--------------
Page 3
Immediate Help for the Uninsured (Interim High-Risk Pool). Immediately creates an insurance program with financial assistance for those who have been uninsured for several months or denied a policy because of preexisting conditions.
Repeals the Antitrust Exemption for Insurers. The bill promotes competition among health insurers and medical malpractice insurers by removing the antitrust exemption so that it no longer shields these insurers from liability for fixing prices, dividing up territories, or monopolizing their market.
I. HEALTH REFORM
Small Employer Exemption. Exempts 86% of small businesses from the requirement to offer or contribute to coverage by increasing the thresholds for exemption from $250,000 of payroll to $500,000; decreases obligations for employers with payrolls between $500,000 and $750,000 by graduating the application of the contribution, so that the full 8 percent contribution level begins at annual payrolls of $750,000 instead of $400,000, as originally proposed in HR 3200.
Small Employers and the Exchange. Increases the size of small employers automatically allowed to purchase coverage through the Exchange to at least 100 employees within the first 3 years; permits additional expansion to even larger employers in future years.
Small Business Tax Credit. Modifies the policy to limit the tax credit to a two-year period per firm to help firms transition to providing health benefits to their employees.
Health Insurance Co-ops. Provides start-up loans to establish not-for-profit or cooperative health plans that compete with private insurers and the public health insurance option. These start-up costs are treated the same as those provided to the public option and are paid back to the federal government by amortizing the loan amount in future premiums.
Veterans and Members of the Armed Forces. Ensures veterans, members of the armed forces, and their families have access to the Exchange to obtain health insurance if they choose and that they fulfill their responsibility to have qualified health insurance if they are enrolled in VA healthcare or TRICARE. Also
provides that TRICARE is not changed based on the essential benefits package.
Essential Benefits Package. Provides for the coverage of behavioral health treatments as mental health services, and clarifies that durable medical equipment, prosthetics, and orthotics are covered in the essential benefits package.
Provider Non-discrimination. Preserves state-enacted provider non-discrimination laws.
Protections for American Indians. Taxpayers who are eligible for health care services as members of a federally-recognized Indian Tribe are treated as having satisfied the individual responsibility requirement. Health coverage that is provided by a tribe to a tribal member is excluded from the tribal member’s taxable income. Standards for qualified health benefit plans, including the public option, are modified to provide for
rules regarding Indian enrollees and Indian health care providers.
------------------
Page 4
Territories. Allows each territory to elect to participate in the Exchange and provides $4 billion in funds for affordability credits if the territory adopts the insurance reforms and requirements for individual and employer responsibility in the bill.
Legal Status Verification. Establishes a mechanism by which the Commissioner must verify that individuals are citizens or legal immigrants in order to receive affordability credits.
Medical Malpractice. Establishes new voluntary state grant program designed to encourage states to implement alternatives (“early offer” or certificate of merit approach) to traditional medical malpractice litigation.
Abortion. Prohibits abortion services from being made part of essential benefits package. Prohibits federal funds from being used to pay for abortion (except in cases of rape, incest, and to save life of the woman). Only private premium dollars can be used to provide abortion coverage. Where abortion coverage is
provided, funds for this purpose must be segregated from other funds, including affordability credits.
State Health Insurance Compacts. Permits states to enter into agreements to allow for the sale of insurance across state lines when the state legislatures of the states in question agree to do so. Provides grants to states to enter into compacts, which could increase insurance choices for consumers in a state.
Advance Care Planning. Requires health insurers in the Exchange to present enrollees with information about resources available for advanced care planning.
Members of Congress and the Public Health Insurance Option. Clarifies that Members of Congress may enroll in the public option.
Comparative Effectiveness Research. Increases the independence of the Comparative Effectiveness Research
Commission: Comptroller General appoints the commission, no longer established by the Secretary of HHS; establishes a separate independent funding stream for the Commission; ensures that the Commission is able to make reports without HHS review. Improves protections to ensure that subpopulations are appropriately accounted for in research study design and implementation and requires a researcher with expertise in racial
and ethnic minority health research to be on the Comparative Effectiveness Research Commission. Clarifies that comparative effectiveness reports are not considered as mandates for payment, coverage or treatment and that no federal officer or employee will interfere with the practice of medicine.
II.. IMMEDIIATE IINVESTMENTS IN HEALTH REFORM
(Described in more detail in immediate investments document)
Limitation on Pre-existing Condition Look-Backs. Prior to the bill’s complete prohibition on pre-existing condition exclusions beginning in 2013, shortens the time that plans can look back for pre-existing conditions from 6 months to 30 days and shortens the time plans may exclude coverage of certain benefits generally
from 12 months to 3 months.
Prohibiting Acts of Domestic Violence from being Treated as a Pre-existing Condition. Prohibits insurers
from limiting or denying coverage based on acts stemming from domestic violence.
------------------
Page 5
Increase Dependent Age for Insurance through 26. Allows individuals through age 26 not otherwise covered to remain on their parents’ health insurance at their parents’ discretion.
COBRA Extension. Allows individuals to keep their COBRA coverage until the Exchange is up and running.
Specifies a Minimum Medical Loss Ratio of 85%. Increases the value of health insurance by requiring insurers to spend at least 85 percent of their premium dollars on medical care (versus administration or overhead and profits) up until the insurance reforms are implemented.
Ban on Lifetime Limits. Prohibits insurance companies from placing lifetime caps on coverage.
Limitation on Post-Retirement Reductions of Retiree Healthcare Benefits. Prohibits employers from reducing retirees’ health benefits after those retirees have retired, unless the reduction is also made to benefits for active participants.
Employer Wellness Programs. Establishes a grant program for small employers to promote healthy behaviors and provide non-discriminatory incentives among their employees.
Reconstructive Surgery for Children. Requires plans to pay for reconstructive surgery for children with deformities.
Grants to States for Immediate Health Reform Initiatives. Builds on an existing grant program to enhance incentives for states to move forward with a variety of health reform initiatives prior to 2013.
III. MEDICARE
Accountable Care Organization and Medical Home Pilot Programs. Requires the Secretary to set specific benchmarks for expansion of these programs and to test them in a variety of settings and geographic regions. If the initial pilots prove successful, the Secretary is directed to continue expanding them on a large scale basis. The scope of participants in the community-based medical home pilot is expanded to potentially include any eligible beneficiary.
Promotes Bundling. Increases opportunity for providers to coordinate care and payment across settings.
Extends Hospice Moratorium. Extends a 1-year moratorium on regulatory changes that would phase out the budget neutrality adjustment factor for hospice providers to ensure that hospices continue to receive the same reimbursement rate for wages for fiscal year 2010.
Clarifies Voluntary Advance Care Planning Benefit. Clarifies and simplifies a voluntary new benefit in Medicare.
Assessment of Cost-Intensive Diseases and Conditions. Requires HHS to periodically assess diseases and conditions that are or could become the most cost-intensive for the Medicare program. This information will be used to help inform research priorities into prevention and treatment strategies conducted at HHS agencies, such as the National Institutes of Health and whether current spending on research into such conditions is appropriate.
-----------------
Page 6
Home Health Study. Requires MedPAC to undertake a study to examine the significant variation in Medicare margins among home health agencies. Factors considered will include patient characteristics (including health and socioeconomic factors), agency characteristics, and the types of services provided by different agencies.
IV. MEDICAID
Medicaid Payment for Primary Care Services. Retains federal matching rate for costs of increasing Medicaid payment rates to Medicare levels at 100% through 2014, then reduces rate to 90% in 2015 and beyond.
Medicaid Preventive Services. Prohibits imposition of cost-sharing on recommended preventive services.
Supplemental Payments to Certain Nursing Facilities. Directs the Secretary to make supplemental payments to skilled nursing facilities with high percentages of Medicare and Medicaid patients and that are efficiently operated and provide quality care. Provides $6 billion over the period 2010 through 2013 for this purpose with no state contribution. Directs the new Medicaid and CHIP Payment and Access Commission (MACPAC) to study the adequacy of Medicaid payments to nursing facilities and to provide recommendations to the Congress by December 31, 2011.
V. LOWERIING DRUG COSTS
Encourages Accurate Dispensing of Drugs. Require that Part D and MA-PD plans develop practices to reduce waste of drugs in the long-term care setting.
Increases Use of Generics. Increases generic drug utilization by eliminating current requirements that prevent Part D and MA-PD plans from paying for and creating incentives for seniors to use lower-cost generic drugs.
Follow-on Biologics. Creates an FDA licensure pathway for "biosimilar" generic biological products, allowing these products to come to market and compete with brand-name biologics. The biosimilar product must have no clinically meaningful differences in safety, purity or potency from the reference product, and may not be licensed until at least 12 years after the date that the brand-name product was licensed.
VI. PUBLIIC HEALTH
Research and Requirements for Healthy Behaviors and Community Wellness. Provides for the research and inclusion of proven healthy behaviors in the essential benefits package and in community wellness programs.
Overweight and Obesity Prevention Program. Establishes a new grants program to prevent overweight and obesity among children.
Autism Training Initiative. Supports training activities to address the unmet needs of children and adults with autism and related developmental disabilities.
----------------
Page 7
Emergency Room and Trauma Center Capacity. Provides grants to strengthen the nation’s emergency room and trauma center capacity.
Telehealth. Reauthorizes grant programs to support telehealth networks and telehealth resource centers, and provides incentives to coordinate telemedicine licensure activities among states.
Training of Mental and Behavioral Health Professionals. Establishes a new training program for mental and behavioral health professionals, including those specializing in substance abuse counseling and addiction medicine, to promote interdisciplinary training and coordination of the delivery of health care.
Expanded Participation in 340B Program. Extends the section 340B outpatient drug discounts to certain rural and other hospitals, including Critical Access Hospitals.
Menu labeling. Requires chain restaurants to put the calorie content of their menu items directly on the menus and to provide other nutritional information available so that consumers can make informed choices about what they eat.
IHS Reauthorization. Reauthorizes the Indian Health Care Improvement Act (IHCIA). IHCIA provides the main legal authority for the provision of health care to American Indians and Alaskan Natives. The last authorization expired in 2001 and legislation to reauthorize IHCIA has been pending before the Congress since 1999. The main provisions of this new division would address: improvements in workforce development and recruitment; facilities construction, maintenance and improvements; access to and financing of health services; provision of health services for urban Indians; organization improvements within the Indian Health Service (IHS); and the provision of behavioral health services.
VII. REVENUES
Additional revenues. Information reporting for payments made to corporations; elimination of nontaxable reimbursements of over the counter medications from HSAs, HRAs, and health FSAs; a $2,500 limit on contributions to health FSAs (indexed to the consumer price index); an increase in the penalty for non-health related distributions from HSAs (from 10 percent to 20 percent); elimination of the tax deduction for employers who receive a government subsidy for providing retiree prescription drug coverage; a 2.5% excise tax on the sale of a medical device for use in the United States (excluding resales and retail sales); and tax parity for employer-provided coverage for domestic partners and other non-dependents.
PREPARED BY THE COMMITTEES ON WAYS & MEANS, ENERGY & COMMERCE, AND EDUCATION & LABOR
OCTOBER 29, 2009"
energycommerce.house.gov/Press_111/health_care/hr3962_TOPLINE.pdf
"
TOPLINE CHANGES FROM INTRODUCED BILL TO BLENDED BILL
This document is a list of the major policy changes between the Affordable Health Care for America Act (10/29/09) from the introduced HR 3200 bill (7/19/09); it does not include every change....
TOP TIER CHANGES....
Modifies the Income Thresholds and Rates for the Surcharge. In the introduced bill, the surcharge applied to adjusted gross income in excess of $350,000 (married filing a joint return) and $280,000 (single), at rates ranging from 1% to 5.4%. Under the blended bill, the surcharge applies to adjusted gross income in excess of $1 million (married filing a joint return) and $500,000 (single), at a rate of 5.4%.
Public Health Insurance Option. Modifies policy so that the Secretary shall negotiate rates with providers that participate in the public plan and provides greater clarity regarding the opt-out policy for providers.
Physician Payment Reform. Removes overhaul of the Medicare physician payment formula (SGR), which will be permanently reformed by separate legislation this year.
Affordability Credits. In order to reduce the cost of the new coverage to meet the $900 billion goal, affordability premium credits have been scaled back to reflect an amendment adopted by the Committee on Energy & Commerce. Individuals and families between 150% and 400% of FPL [Federal Poverty Level] will pay a larger share of health premiums over time compared to HR 3200 as introduced. Also, the exception for individuals and families with employer coverage who can receive affordability credits in the Exchange is increased to 12% of income. Specific out-of-pocket maximums are added to protect individuals’ level of cost sharing at each income tier (specified below).
----------------------
Page 2

Medicaid. Raises threshold for mandatory Medicaid coverage from 133% of poverty to 150%. Retains 100% federal matching rate for costs of expansion populations in 2013 and 2014, then reduces rate to 91 percent in 2015 and beyond. Deletes provision allowing recently uninsured childless adults with incomes under 133% of poverty to choose between Medicaid and the Exchange. Increases assistance to states that maintain access to Medicaid services during the recession by extending the current Recovery Act increase in federal Medicaid payments to states with high unemployment rates.
Begins Closing the Medicare Part D Donut Hole Immediately. Effective January 1, 2010, closes the Part D donut hole by $500 and institutes a 50% discount for brand-name drugs in the donut hole. Gap in coverage is completely eliminated by 2019.
Secretarial Negotiation of Drug Prices in Medicare. Secretary of HHS is required to negotiate drug prices on
behalf of Medicare beneficiaries.
Addresses Geographic Variation in Health Spending. Instructs the IOM to study the extent and cause of geographic variation in spending on health care (including all payers). The study will focus on major contributors to that variation such as input prices, health status, socioeconomic factors, and access to services. The IOM will make recommendations to the Secretary, and the Secretary will submit to the Congress an implementation plan to appropriately address such variation in Medicare. To the extent the plan would result in dramatically different payments, it must take into account the need to maintain beneficiary access to
services and minimize disruption for providers. CMS will implement changes to Medicare payment systems unless Congress votes to disapprove the planned changes.
Establishes a Center for Medicare & Medicaid Innovation. Creates a Center for Medicare & Medicaid Payment Innovation within CMS not later than 2011 to test and expand new payment models that encourage higher quality and lower cost.
CLASS Act. Creates a new, voluntary, public, long-term care insurance program to help purchase services and supports for people who have functional limitations. After a contribution period, individuals determined to need assistance because of functional limitations would qualify to receive a daily or weekly cash benefit to help purchase the services and supports needed to maintain personal and financial independence. CLASS would supplement, not supplant, traditional payers of long-term care (e.g. Medicaid and/or private long term care insurance).
Immediate Sunshine on Price Gouging (Rate Review). Discourages excessive price increases by insurance companies through review and disclosure of insurance rate increases and rationale for such increases.
--------------
Page 3
Immediate Help for the Uninsured (Interim High-Risk Pool). Immediately creates an insurance program with financial assistance for those who have been uninsured for several months or denied a policy because of preexisting conditions.
Repeals the Antitrust Exemption for Insurers. The bill promotes competition among health insurers and medical malpractice insurers by removing the antitrust exemption so that it no longer shields these insurers from liability for fixing prices, dividing up territories, or monopolizing their market.
I. HEALTH REFORM
Small Employer Exemption. Exempts 86% of small businesses from the requirement to offer or contribute to coverage by increasing the thresholds for exemption from $250,000 of payroll to $500,000; decreases obligations for employers with payrolls between $500,000 and $750,000 by graduating the application of the contribution, so that the full 8 percent contribution level begins at annual payrolls of $750,000 instead of $400,000, as originally proposed in HR 3200.
Small Employers and the Exchange. Increases the size of small employers automatically allowed to purchase coverage through the Exchange to at least 100 employees within the first 3 years; permits additional expansion to even larger employers in future years.
Small Business Tax Credit. Modifies the policy to limit the tax credit to a two-year period per firm to help firms transition to providing health benefits to their employees.
Health Insurance Co-ops. Provides start-up loans to establish not-for-profit or cooperative health plans that compete with private insurers and the public health insurance option. These start-up costs are treated the same as those provided to the public option and are paid back to the federal government by amortizing the loan amount in future premiums.
Veterans and Members of the Armed Forces. Ensures veterans, members of the armed forces, and their families have access to the Exchange to obtain health insurance if they choose and that they fulfill their responsibility to have qualified health insurance if they are enrolled in VA healthcare or TRICARE. Also
provides that TRICARE is not changed based on the essential benefits package.
Essential Benefits Package. Provides for the coverage of behavioral health treatments as mental health services, and clarifies that durable medical equipment, prosthetics, and orthotics are covered in the essential benefits package.
Provider Non-discrimination. Preserves state-enacted provider non-discrimination laws.
Protections for American Indians. Taxpayers who are eligible for health care services as members of a federally-recognized Indian Tribe are treated as having satisfied the individual responsibility requirement. Health coverage that is provided by a tribe to a tribal member is excluded from the tribal member’s taxable income. Standards for qualified health benefit plans, including the public option, are modified to provide for
rules regarding Indian enrollees and Indian health care providers.
------------------
Page 4
Territories. Allows each territory to elect to participate in the Exchange and provides $4 billion in funds for affordability credits if the territory adopts the insurance reforms and requirements for individual and employer responsibility in the bill.
Legal Status Verification. Establishes a mechanism by which the Commissioner must verify that individuals are citizens or legal immigrants in order to receive affordability credits.
Medical Malpractice. Establishes new voluntary state grant program designed to encourage states to implement alternatives (“early offer” or certificate of merit approach) to traditional medical malpractice litigation.
Abortion. Prohibits abortion services from being made part of essential benefits package. Prohibits federal funds from being used to pay for abortion (except in cases of rape, incest, and to save life of the woman). Only private premium dollars can be used to provide abortion coverage. Where abortion coverage is
provided, funds for this purpose must be segregated from other funds, including affordability credits.
State Health Insurance Compacts. Permits states to enter into agreements to allow for the sale of insurance across state lines when the state legislatures of the states in question agree to do so. Provides grants to states to enter into compacts, which could increase insurance choices for consumers in a state.
Advance Care Planning. Requires health insurers in the Exchange to present enrollees with information about resources available for advanced care planning.
Members of Congress and the Public Health Insurance Option. Clarifies that Members of Congress may enroll in the public option.
Comparative Effectiveness Research. Increases the independence of the Comparative Effectiveness Research
Commission: Comptroller General appoints the commission, no longer established by the Secretary of HHS; establishes a separate independent funding stream for the Commission; ensures that the Commission is able to make reports without HHS review. Improves protections to ensure that subpopulations are appropriately accounted for in research study design and implementation and requires a researcher with expertise in racial
and ethnic minority health research to be on the Comparative Effectiveness Research Commission. Clarifies that comparative effectiveness reports are not considered as mandates for payment, coverage or treatment and that no federal officer or employee will interfere with the practice of medicine.
II.. IMMEDIIATE IINVESTMENTS IN HEALTH REFORM
(Described in more detail in immediate investments document)
Limitation on Pre-existing Condition Look-Backs. Prior to the bill’s complete prohibition on pre-existing condition exclusions beginning in 2013, shortens the time that plans can look back for pre-existing conditions from 6 months to 30 days and shortens the time plans may exclude coverage of certain benefits generally
from 12 months to 3 months.
Prohibiting Acts of Domestic Violence from being Treated as a Pre-existing Condition. Prohibits insurers
from limiting or denying coverage based on acts stemming from domestic violence.
------------------
Page 5
Increase Dependent Age for Insurance through 26. Allows individuals through age 26 not otherwise covered to remain on their parents’ health insurance at their parents’ discretion.
COBRA Extension. Allows individuals to keep their COBRA coverage until the Exchange is up and running.
Specifies a Minimum Medical Loss Ratio of 85%. Increases the value of health insurance by requiring insurers to spend at least 85 percent of their premium dollars on medical care (versus administration or overhead and profits) up until the insurance reforms are implemented.
Ban on Lifetime Limits. Prohibits insurance companies from placing lifetime caps on coverage.
Limitation on Post-Retirement Reductions of Retiree Healthcare Benefits. Prohibits employers from reducing retirees’ health benefits after those retirees have retired, unless the reduction is also made to benefits for active participants.
Employer Wellness Programs. Establishes a grant program for small employers to promote healthy behaviors and provide non-discriminatory incentives among their employees.
Reconstructive Surgery for Children. Requires plans to pay for reconstructive surgery for children with deformities.
Grants to States for Immediate Health Reform Initiatives. Builds on an existing grant program to enhance incentives for states to move forward with a variety of health reform initiatives prior to 2013.
III. MEDICARE
Accountable Care Organization and Medical Home Pilot Programs. Requires the Secretary to set specific benchmarks for expansion of these programs and to test them in a variety of settings and geographic regions. If the initial pilots prove successful, the Secretary is directed to continue expanding them on a large scale basis. The scope of participants in the community-based medical home pilot is expanded to potentially include any eligible beneficiary.
Promotes Bundling. Increases opportunity for providers to coordinate care and payment across settings.
Extends Hospice Moratorium. Extends a 1-year moratorium on regulatory changes that would phase out the budget neutrality adjustment factor for hospice providers to ensure that hospices continue to receive the same reimbursement rate for wages for fiscal year 2010.
Clarifies Voluntary Advance Care Planning Benefit. Clarifies and simplifies a voluntary new benefit in Medicare.
Assessment of Cost-Intensive Diseases and Conditions. Requires HHS to periodically assess diseases and conditions that are or could become the most cost-intensive for the Medicare program. This information will be used to help inform research priorities into prevention and treatment strategies conducted at HHS agencies, such as the National Institutes of Health and whether current spending on research into such conditions is appropriate.
-----------------
Page 6
Home Health Study. Requires MedPAC to undertake a study to examine the significant variation in Medicare margins among home health agencies. Factors considered will include patient characteristics (including health and socioeconomic factors), agency characteristics, and the types of services provided by different agencies.
IV. MEDICAID
Medicaid Payment for Primary Care Services. Retains federal matching rate for costs of increasing Medicaid payment rates to Medicare levels at 100% through 2014, then reduces rate to 90% in 2015 and beyond.
Medicaid Preventive Services. Prohibits imposition of cost-sharing on recommended preventive services.
Supplemental Payments to Certain Nursing Facilities. Directs the Secretary to make supplemental payments to skilled nursing facilities with high percentages of Medicare and Medicaid patients and that are efficiently operated and provide quality care. Provides $6 billion over the period 2010 through 2013 for this purpose with no state contribution. Directs the new Medicaid and CHIP Payment and Access Commission (MACPAC) to study the adequacy of Medicaid payments to nursing facilities and to provide recommendations to the Congress by December 31, 2011.
V. LOWERIING DRUG COSTS
Encourages Accurate Dispensing of Drugs. Require that Part D and MA-PD plans develop practices to reduce waste of drugs in the long-term care setting.
Increases Use of Generics. Increases generic drug utilization by eliminating current requirements that prevent Part D and MA-PD plans from paying for and creating incentives for seniors to use lower-cost generic drugs.
Follow-on Biologics. Creates an FDA licensure pathway for "biosimilar" generic biological products, allowing these products to come to market and compete with brand-name biologics. The biosimilar product must have no clinically meaningful differences in safety, purity or potency from the reference product, and may not be licensed until at least 12 years after the date that the brand-name product was licensed.
VI. PUBLIIC HEALTH
Research and Requirements for Healthy Behaviors and Community Wellness. Provides for the research and inclusion of proven healthy behaviors in the essential benefits package and in community wellness programs.
Overweight and Obesity Prevention Program. Establishes a new grants program to prevent overweight and obesity among children.
Autism Training Initiative. Supports training activities to address the unmet needs of children and adults with autism and related developmental disabilities.
----------------
Page 7
Emergency Room and Trauma Center Capacity. Provides grants to strengthen the nation’s emergency room and trauma center capacity.
Telehealth. Reauthorizes grant programs to support telehealth networks and telehealth resource centers, and provides incentives to coordinate telemedicine licensure activities among states.
Training of Mental and Behavioral Health Professionals. Establishes a new training program for mental and behavioral health professionals, including those specializing in substance abuse counseling and addiction medicine, to promote interdisciplinary training and coordination of the delivery of health care.
Expanded Participation in 340B Program. Extends the section 340B outpatient drug discounts to certain rural and other hospitals, including Critical Access Hospitals.
Menu labeling. Requires chain restaurants to put the calorie content of their menu items directly on the menus and to provide other nutritional information available so that consumers can make informed choices about what they eat.
IHS Reauthorization. Reauthorizes the Indian Health Care Improvement Act (IHCIA). IHCIA provides the main legal authority for the provision of health care to American Indians and Alaskan Natives. The last authorization expired in 2001 and legislation to reauthorize IHCIA has been pending before the Congress since 1999. The main provisions of this new division would address: improvements in workforce development and recruitment; facilities construction, maintenance and improvements; access to and financing of health services; provision of health services for urban Indians; organization improvements within the Indian Health Service (IHS); and the provision of behavioral health services.
VII. REVENUES
Additional revenues. Information reporting for payments made to corporations; elimination of nontaxable reimbursements of over the counter medications from HSAs, HRAs, and health FSAs; a $2,500 limit on contributions to health FSAs (indexed to the consumer price index); an increase in the penalty for non-health related distributions from HSAs (from 10 percent to 20 percent); elimination of the tax deduction for employers who receive a government subsidy for providing retiree prescription drug coverage; a 2.5% excise tax on the sale of a medical device for use in the United States (excluding resales and retail sales); and tax parity for employer-provided coverage for domestic partners and other non-dependents.
PREPARED BY THE COMMITTEES ON WAYS & MEANS, ENERGY & COMMERCE, AND EDUCATION & LABOR
OCTOBER 29, 2009"
